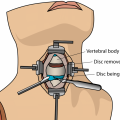
Cervical disc disease describes the degenerative process in the cervical spine discs. Usually, cervical disc disease Roswell develops as the discs between each vertebra start to break down due to wear and tear. Most people with cervical degenerative disease experience neck pain and radiating arm pain. While anyone can develop cervical disc disease, genetic components predispose some people to more rapid wear, and sometimes an injury can cause or accelerate degenerative changes.
Disc degeneration process
The spine is made up of a series of vertebrae, and in between each bone lies a disc that cushions the vertebral bones, preventing them from rubbing against each other; they also act as shock absorbers and hold the spine in position. Each disc has a tough but flexible outer membrane of woven cartilage strands called the annulus fibrosus and a soft interior filled with a mucoprotein gel called the nucleus pulposus.
Discs are usually hydrated; in children, discs are about 85% water. However, as you grow older, discs dry out, providing less cushioning and becoming prone to cracks and tears. The disc’s water content drops to 70% by the time you are 70, but in some people, the disc dehydration is more rapid. Over time, discs may not be able to repair themselves because of indirect blood supply. As such, a tear in the disc’s outer membrane will not heal or will develop weak scar tissue, which can break again.
The course of cervical degenerative disc disease
Cervical disc disease is technically not a disease but a description of the age-related wear and tear in the cervical spine discs. Almost everyone who lives long enough will develop degenerative discs. Most adults with degenerative disc disease have no symptoms, despite a higher percentage showing signs of disc degeneration in imaging tests, including MRI. Disc degeneration can occur as soon as the early 20s, but it is more prevalent in people who are 50 years and older.
However, sometimes the cervical degenerative disease can cause pain in various ways; in some cases, the disc itself becomes painful. Discogenic pain is most likely to occur in people between their 30s and 50s. When cervical degenerative disc disease symptoms become chronic, they are likely to stem from other conditions such as osteoarthritis, herniated disc, or spinal stenosis. The pain may be acute or chronic depending on the cause; for example, pain from a ruptured disc may not need medical intervention, but osteoarthritis may require long-term treatment.
Risk factors for cervical disc disease
Although almost everyone ultimately gets cervical degenerative disc disease as they age, some factors may make you more likely to become symptomatic or develop degenerative disc disease sooner. Examples of these risk factors include:
- Obesity. Excess body weight causes added pressure on your vertebral bones, pressing on the discs and accelerating wear and tear. Therefore, it is essential to lose extra weight and stay within your ideal weight.
- Genetics. Genetics factors may cause you to develop disc degeneration earlier than usual.
- Smoking. Smoking narrows blood vessels, limiting blood and nutrient supply to the discs, making them lose hydration more quickly.
Consult your healthcare provider at Polaris Spine & Neurosurgery Center to learn about treatment options for cervical disc disease.