Let’s be honest. The convenience of telemedicine is incredible. From your couch, you can see a doctor for a sinus infection, get therapy, or manage a chronic condition. It saves time, reduces stress, and honestly, feels a bit like the future. But that future hits a snag when the bill arrives and you’re left wondering, “Will my insurance cover this?”
Here’s the deal: insurance reimbursement policies for telehealth have evolved dramatically, especially since 2020. They’re no longer a fringe benefit. But the landscape is a patchwork—complex, shifting, and sometimes downright confusing. This guide will walk you through what you need to know to navigate it confidently.
The New Normal: How Insurance Views Telehealth Now
Gone are the days when telemedicine was a rare, cash-only novelty. The pandemic blew the doors open, and most major insurers—Medicare, Medicaid, and private carriers—have kept them at least partway open. But it’s not a uniform policy. Think of it like streaming services: the basic package might cover a video visit with your primary doctor, but the premium plan is needed for a specialist in another state.
Permanent changes are still being cemented by state and federal laws. So, while coverage is broadly available, the specifics? They hinge on a few key factors.
Key Factors That Determine Your Telehealth Coverage
Not all virtual visits are created equal in the eyes of your insurer. These are the main levers that affect reimbursement:
- Your Insurance Plan Type: This is the big one. Private employer plans, ACA marketplace plans, Medicare, and Medicaid all have different rules. A plan from 2024 is far more likely to have embedded telehealth benefits than one from 2018.
- Your State of Residence: Insurance is state-regulated. Over 40 states have some form of telemedicine parity laws. These laws generally require insurers to cover telehealth services at the same rate (parity) as in-person care. But the strength of these laws varies—a lot.
- The Type of Service Provided: A routine follow-up for a known condition? Usually covered. Mental health counseling? Increasingly standard. Physical therapy via video? That’s trickier. Some services require a physical component that’s hard to replicate virtually.
- The Technology Used: Most insurers now cover visits conducted via live, interactive video (like Zoom or a secure platform). Reimbursement for audio-only phone calls or asynchronous “store-and-forward” messaging is less common, though some states mandate it for certain services.
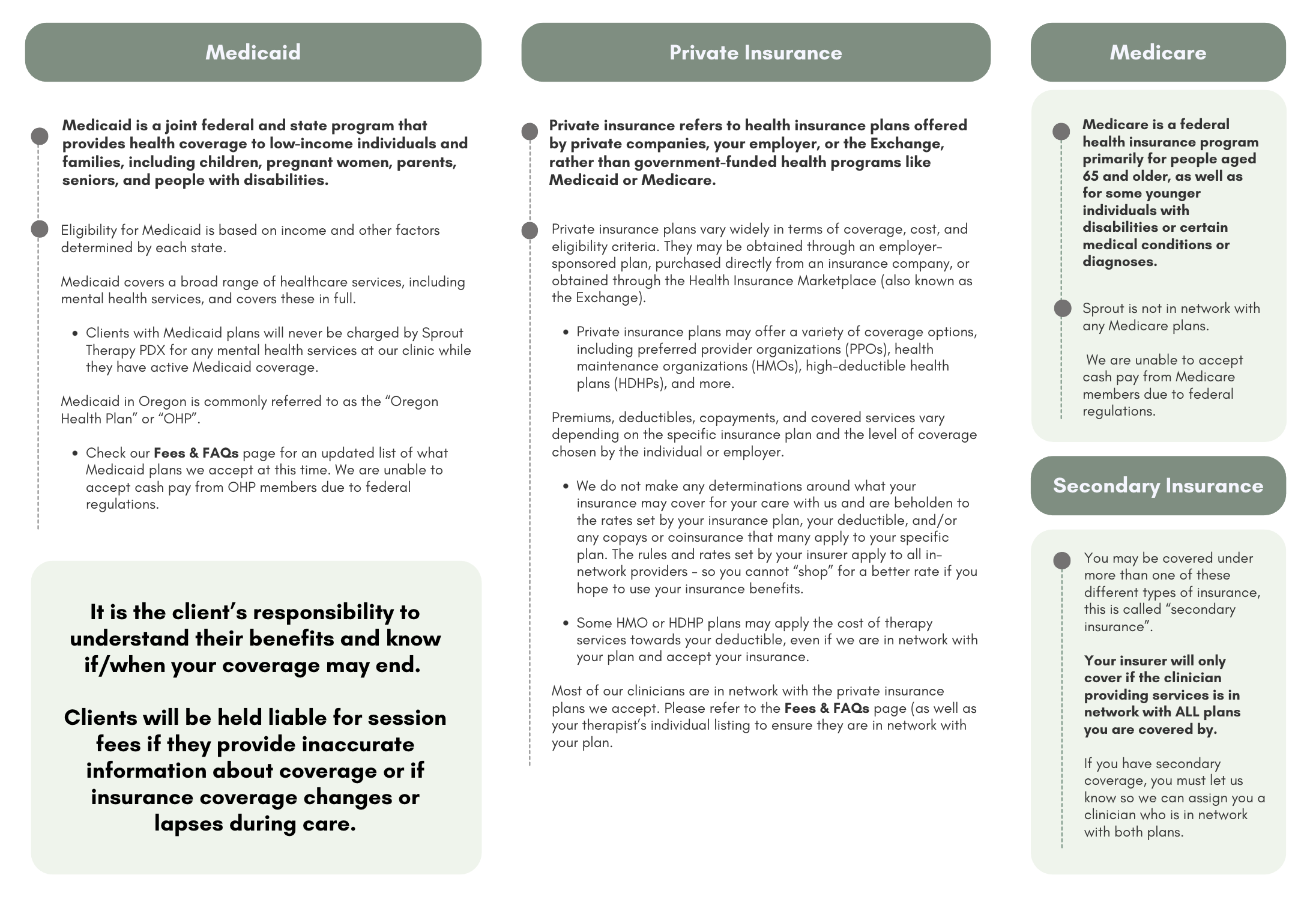
Decoding the Major Players: Medicare, Medicaid, and Private Insurance
Let’s break down the big three. This is where you’ll find the core of your answer.
Medicare Telehealth Reimbursement Policies
Medicare’s telehealth expansion was temporary, but Congress has extended it repeatedly. As of now, beneficiaries can use telehealth from anywhere, including their home—not just a rural clinic. The originating site restriction, a huge barrier, is waived. Covered services include office visits, psychotherapy, and certain preventive screenings.
Private Insurance and Telemedicine Parity
Most private insurers have embraced telehealth. In states with strong parity laws, they must reimburse it at the same rate as an in-person visit. You’ll often pay your standard copay or coinsurance. Many insurers also offer direct-to-consumer telehealth apps (like Teladoc included in your plan) as a low-cost or $0 option. But here’s the catch: using an out-of-network telehealth provider can lead to surprise bills. Always, always check network status first.
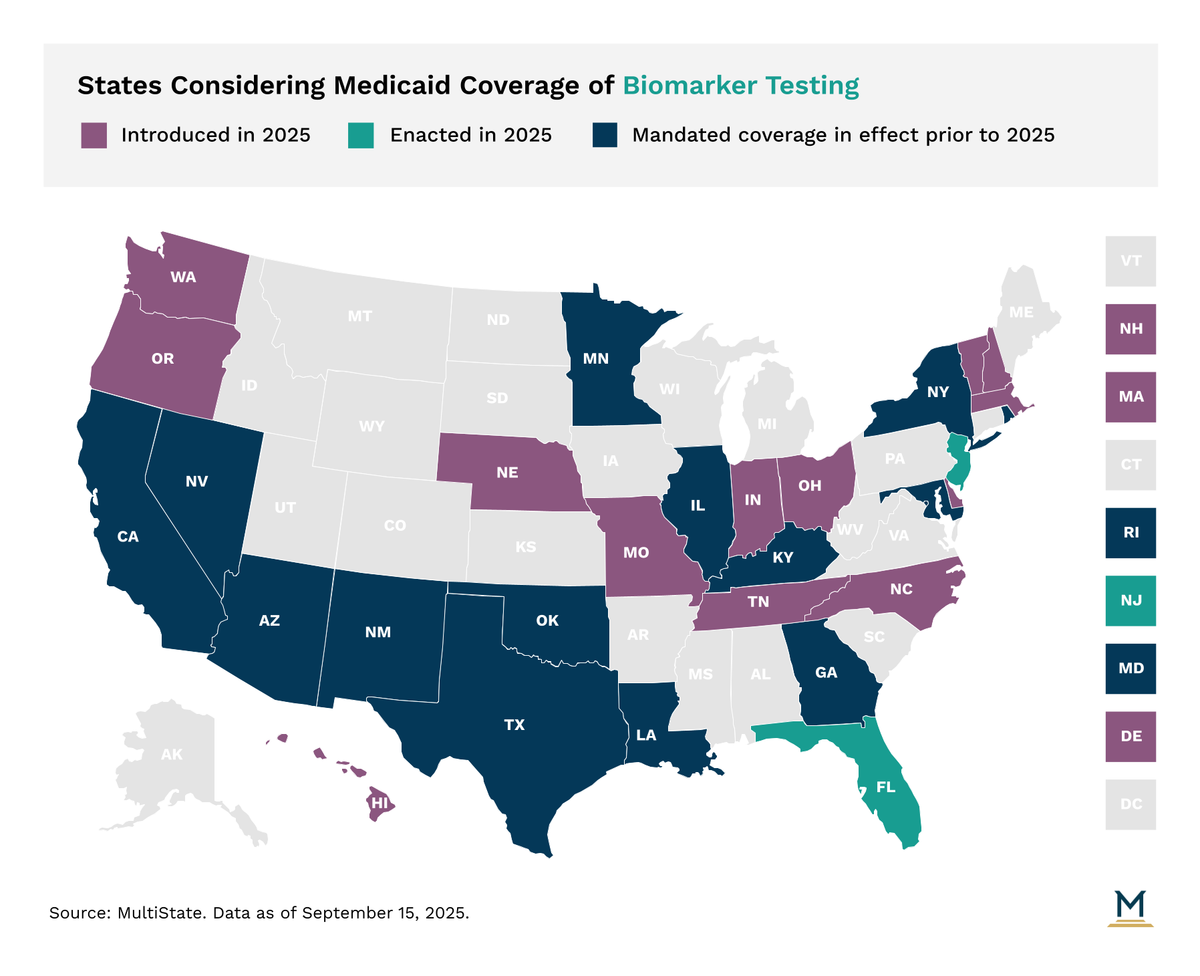
Medicaid Coverage by State
Medicaid is the wild card because it’s administered state-by-state. All 50 states and D.C. cover some form of telehealth, but what’s covered differs wildly. Some states are pioneers, covering a wide range of services, including remote patient monitoring. Others offer the bare minimum. You must check with your specific state Medicaid program.
Actionable Steps: How to Ensure You Get Reimbursed
Don’t leave it to chance. A little legwork prevents headaches later. Follow this checklist:
- Read Your Plan’s Summary of Benefits and Coverage (SBC). Search for terms like “telehealth,” “virtual care,” or “remote services.”
- Call Your Insurer. Ask directly: “Does my plan cover telehealth for [your specific need]? Is there a copay? Do I need a referral or prior authorization?” Get a reference number for the call.
- Verify with Your Provider. Ask your doctor’s office if they are set up for billing telehealth and if they accept your insurance for virtual visits. Not all are.
- Understand the Platform. Confirm the visit will use approved technology (usually interactive video). A simple phone call might not be billable.
- Keep Records. Save all explanation of benefits (EOBs) and bills. If a claim is denied, you’ll need them to appeal.
Common Hiccups and How to Handle Them
Even when you do everything right, things can go sideways. A denied claim isn’t always the end. Common reasons for denial include the service being deemed “not medically necessary” for a virtual format, or a coding error by the provider’s billing staff. If you get a denial, appeal it. Reference the notes from your initial call to the insurer. Patient advocacy works.
Another pain point? The digital divide. Some policies still require a video-capable device, which can exclude patients who only have a landline. Thankfully, this is slowly changing as audio-only proves vital for accessibility.
The Road Ahead: What’s Next for Telehealth Reimbursement?
The trend is clear: telehealth is becoming a staple, not a substitute. Reimbursement policies are stabilizing, but the fight is for permanent parity and expanded services. We’re likely to see more coverage for hybrid care models—where in-person and virtual visits are woven together seamlessly for chronic disease management.
The bottom line? Telemedicine has proven its worth. It’s efficient, patient-centered, and here to stay. And while the insurance maze can be frustrating, understanding the rules of the game empowers you to access care on your terms. You just have to learn how to navigate the system—like any other important journey, a good map makes all the difference.