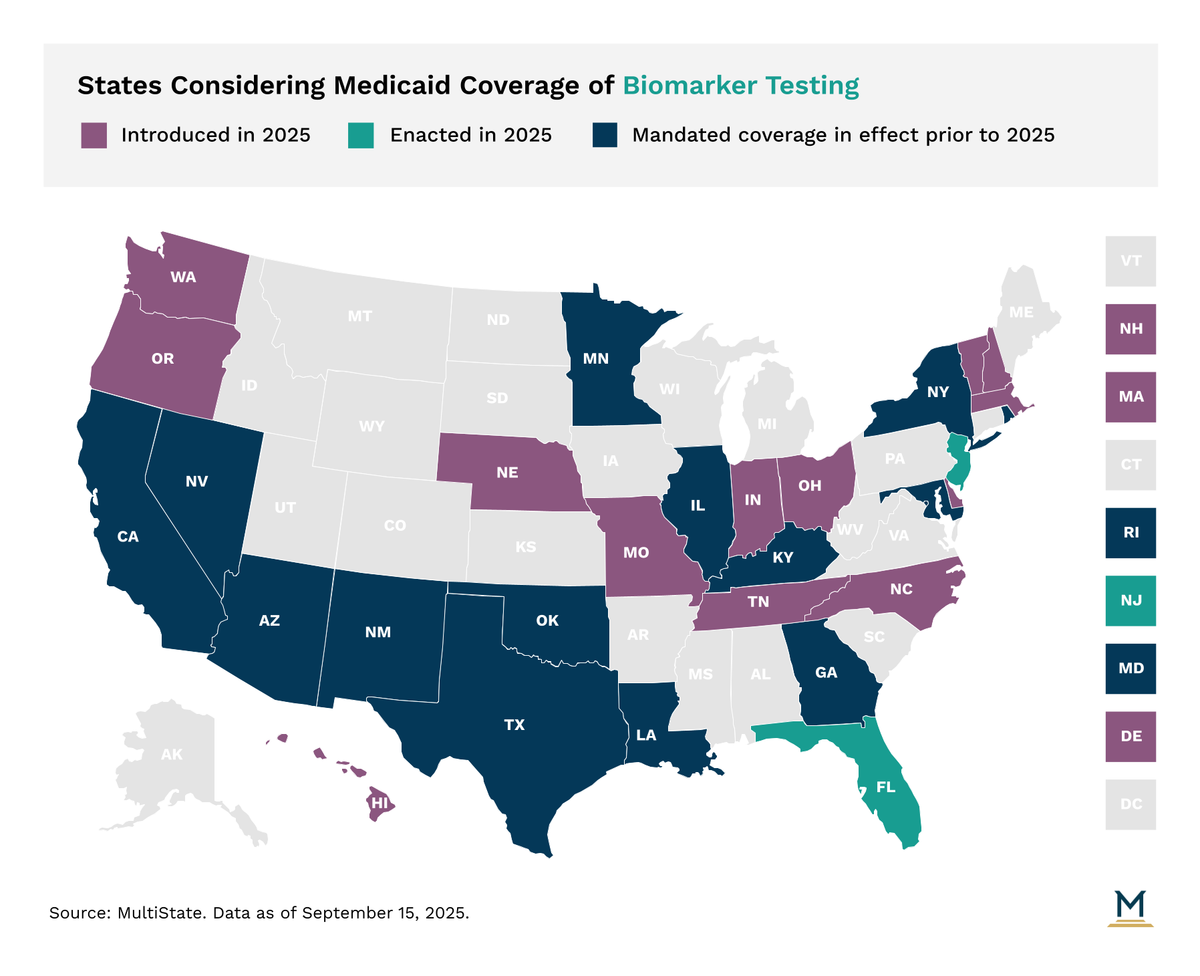
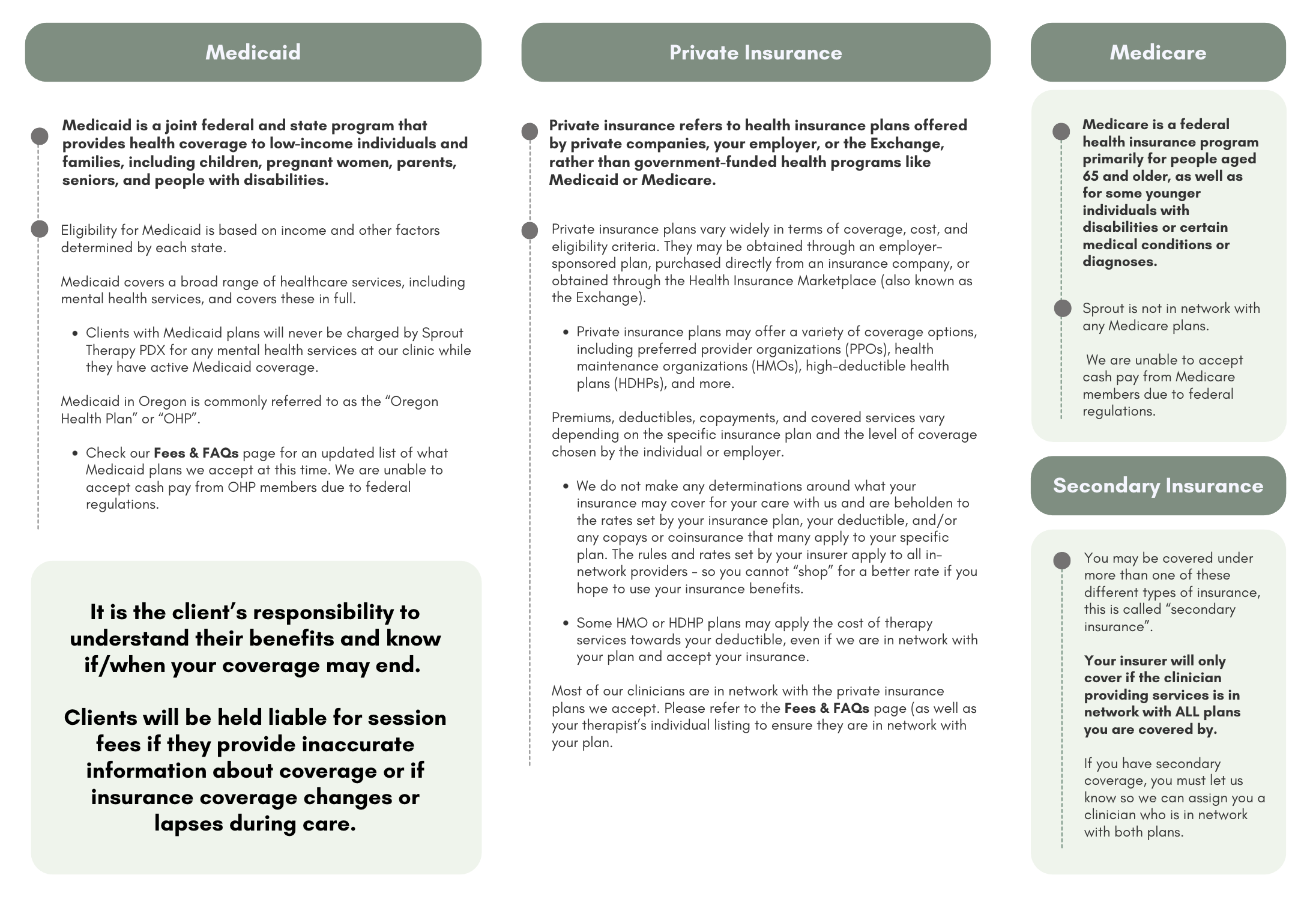
Let’s be honest. The world of health insurance can feel like a maze. You hear about amazing advances in preventative care—especially genetic testing—and wonder, “Is this covered?” Well, the answer is getting clearer, but it’s not a simple yes or no. It’s a shifting landscape, and understanding it is key to taking control of your health.
Here’s the deal: modern health plans are slowly, sometimes awkwardly, adapting to a new era of medicine. An era where we can peek at our genetic blueprint to predict, prevent, and personalize care. But coverage? That’s where the rubber meets the road.
The New Frontier: From Reactive to Proactive Medicine
For decades, health insurance was built on a sick-care model. You get sick, you get treated. Preventative care was basic—yearly physicals, standard vaccines. But genetic testing flips the script. It’s like getting the owner’s manual for your body before the warning light comes on.
This shift is huge. And honestly, it’s what many of us want. We’re not just patients; we’re proactive participants. The challenge is getting our health plans to see it that way too.
When Does Insurance Cover Genetic Testing?
Coverage typically hinges on two things: medical necessity and preventative care guidelines. It’s rarely about curiosity. Most plans follow the lead of major authorities like the U.S. Preventive Services Task Force (USPSTF).
The “Gold Standard” for Coverage
If a test has a high USPSTF recommendation, coverage is almost a given. The big one? BRCA testing for hereditary breast and ovarian cancer risk in women with a specific family history. This is a classic example of preventative care coverage that can literally be life-saving.
Other commonly covered scenarios include:
- Prenatal carrier screening for conditions like cystic fibrosis or Tay-Sachs.
- Pharmacogenetic testing in certain clinical psychiatry or cardiology settings—think figuring out which blood thinner or antidepressant your body will metabolize best.
- Diagnostic testing for individuals with symptoms pointing to a possible genetic condition.
The Gray Areas (And There Are Plenty)
This is where it gets fuzzy. What about multi-gene panels for broader cancer risk? Or whole exome sequencing when other tests fail? Coverage is often a battle, requiring pre-authorization and detailed letters from your doctor.
And then there’s the elephant in the room: direct-to-consumer (DTC) tests like 23andMe or AncestryDNA. Sure, you can learn about your ancestry. But the health reports? Most plans won’t touch them with a ten-foot pole. They’re considered informational, not medically necessary. If a DTC test flags something and you need a clinical-grade test to confirm it, that subsequent test might be covered. It’s a two-step process, you know?
Navigating Your Plan: A Practical Checklist
Don’t fly blind. Before considering any genetic testing for preventative care, do this:
- Talk to Your Doctor. This is non-negotiable. A healthcare provider must establish medical necessity and order the test.
- Decode Your Policy. Look for terms like “genetic testing,” “preventative services,” and “laboratory services” in your Summary of Benefits and Coverage (SBC).
- Call Your Insurer. Ask specific questions: Is this specific CPT code covered? What are the pre-authorization requirements? Which labs are in-network?
- Ask About “Preventative Care” vs. “Diagnostic” Coding. How your doctor codes the test can change your cost from $0 to thousands.
- Get Cost Estimates in Writing. For the test itself, the genetic counseling, and any follow-up.
The Cost Breakdown: What You Might Pay
Even with coverage, costs vary wildly. It’s a mix of deductibles, co-insurance, and lab contracts. Here’s a rough, simplified look at potential scenarios:
| Test Type | Typical Coverage Scenario | Potential Patient Cost* |
|---|---|---|
| BRCA Testing (with family history) | Often fully covered as preventative care | $0 copay, if criteria met |
| Prenatal Carrier Screening | Widely covered, but panel size matters | $0 – $250+ |
| Multi-Gene Cancer Panel | Case-by-case, often requires pre-auth | Deductible & co-insurance may apply (e.g., 20% of $2,000) |
| Direct-to-Consumer Health Test | Rarely, if ever, covered | Full retail price ($99 – $399) |
*This is a general illustration. Your actual costs depend entirely on your plan.
The Future Is Personal (But Is Insurance Ready?)
We’re heading toward a world where your care is tailored to your genes. That’s the promise. The gap is in the payment model. Insurance companies are, understandably, cautious. They need evidence that a test leads to a concrete, cost-effective action.
Does finding a genetic risk for diabetes lead to preventative lifestyle changes that save money long-term? The data says yes, but translating that into blanket coverage is slow. It’s a cultural and financial shift, not just a technological one.
So, where does that leave you? Empowered, but with homework. The system isn’t perfect. It might feel like you’re navigating a frontier. But by understanding the rules—the medical necessity, the codes, the checklist—you can advocate for the preventative care that modern science allows.
In the end, it’s about partnership. With your doctor, with your insurer, and with the unique map your DNA provides. The coverage is evolving because the science already has. And that, honestly, is the most hopeful part of all.