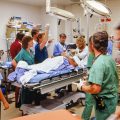
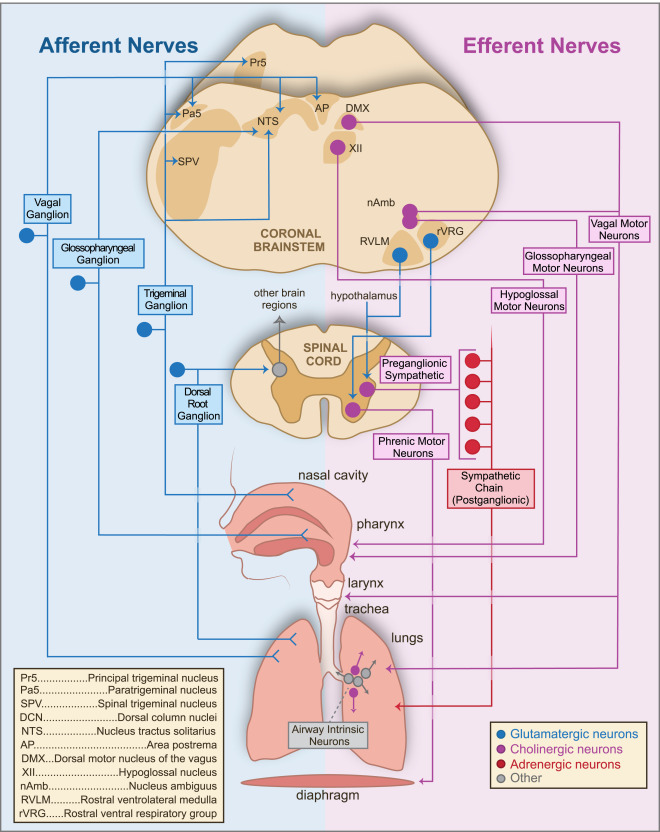
Whether you have a kidney disorder or not, you need to understand the different types of dialysis services offered. For example, there are peritoneal dialysis, hemodialysis, and out-of-center dialysis. In addition, you need to know about the different multimorbidities the dialysis population faces.
Shared decision-making
Almost 30 million Americans have chronic kidney disease, making shared decision-making an essential part of their health care. Shared decision-making involves patients, healthcare professionals, family members, friends, and caregivers in a process that allows the patient to weigh all of their options and make the best decision for them.
Shared decision-making involves a patient’s personal preferences and values in choosing a treatment option. The final decision is based on a balance of the patient’s preferences, deals, and the physician’s medical knowledge.
Many healthcare professionals believe that shared decision-making is essential to patient-centered care. Further, they believe that shared decision-making is a crucial driver for enhancing patient outcomes in chronic conditions. However, some providers need help implementing shared decision-making in practice.
The healthcare industry has taken notice of the importance of shared decision-making in patient care and is working to educate more providers about the concept. In response, the National Quality Forum (NQF) has issued a series of playbooks to help providers implement shared decision-making.
Haemodialysis
Whether you’re considering hemodialysis, you’ve been told that you need it, or you’re already in the process, it’s essential to understand how it works. It is a procedure that enables you to maintain the proper mineral balance in your blood and may prolong your life. But it’s not a cure for kidney failure.
It’s also a way to help control your blood pressure. You’ll need to have blood test results taken every few months to monitor your kidney function and the appropriate prescription for your dialysis. You may need a kidney transplant if you have no kidneys.
Hemodialysis is a process that uses two needles to remove toxins and extra fluids from your blood. It’s often performed in a dialysis center, but you can also do it at home.
Peritoneal dialysis
Performing peritoneal dialysis at home is an excellent option for many people, but there are also some potential benefits and drawbacks. Before you start a peritoneal dialysis program, you should learn how to do each step of the process correctly. In addition, there is a possibility that you might get an infection, although the majority of side effects are treatable.
An infection at the catheter site, or peritonitis, is one of the most common peritoneal dialysis complications. If you do not treat it promptly, it can become severe. Some of the symptoms of peritonitis include fever, swelling, pain, and nausea.
To prevent infections at the catheter site, you should keep it clean. You should also wear a surgical mask and wash your hands often. You should also use an antibiotic to prevent infection.
Out-of-center dialysis
Hundreds of thousands of Americans with kidney failure flock to clinics three times a week for treatment. The number of people needing dialysis increased due to the aging population and the prevalence of hypertension and diabetes.
Medicare pays for end-stage renal disease care. It includes dialysis and kidney transplants. In 2018, Medicare paid $31.3 billion in fee-for-service expenditures for dialysis patients. It is a large chunk of Medicare’s total spending.
Medicare spent 7.2 percent of its total expenditures on kidney failure patients. These patients are often in need of expensive prescription medications. In addition to the prescriptions, patients need dialysis machines. Home hemodialysis is also growing.
Medicare has been leading the charge in payment model reforms for chronic kidney disease. The End-Stage Renal Disease Treatment Choices (ETC) model is the largest experiment in American healthcare history. This incentive system was designed to encourage facilities to offer reasonable home dialysis rates and improve treatment options. The ETC model also provides incentives for increasing the use of home dialysis and promoting living kidney transplantation.
Multimorbidities in the dialysis population
Multimorbidity among chronic kidney disease (CKD) patients is common. Studies have shown that multimorbidity increases treatment burden and adverse clinical outcomes. However, several factors may reduce the treatment burden.
For example, patients with CKD may receive care from multiple specialists. In addition, many patients with CKD also have diabetes. These two conditions are typically treated separately. However, they may also exacerbate each other. Patients with CKD also have other medical conditions, such as hypertension, heart disease, and pulmonary disease. Managing these conditions is essential for improving quality of life.
The number of CKD patients is predicted to increase as the population ages. Multimorbidity challenges are challenging the future of this patient population. This population has a high risk for poor health outcomes and mortality. A better understanding of multimorbidity is essential for adapting healthcare systems.